Have you ever noticed your cat vomiting frequently (more than three times a week), or having stools that contain mucus, traces of blood, or intestinal lining? Perhaps your cat’s weight has been slowly dropping, and their energy level is not what it used to be. These symptoms may seem minor at first, but they can be early warning signs of feline inflammatory bowel disease (IBD).
IBD is not a single, simple illness. It is a complex group of gastrointestinal disorders with varied causes and symptoms. In some cats, inflammatory cells infiltrate the stomach or intestinal wall, causing thickening of the lining and impairing nutrient absorption. Over time, this can lead to malnutrition, weight loss, and overall decline in body condition. Let’s take a closer look at feline inflammatory bowel disease (IBD).
What Is Feline Inflammatory Bowel Disease?
Feline inflammatory bowel disease (IBD) is a chronic gastrointestinal disorder and one of the more common conditions seen in cats. It occurs when the intestinal immune system mounts an abnormal response to normally harmless substances such as food components or intestinal bacteria. The disease is characterized by chronic, persistent, intermittent, or recurring clinical signs.
Under normal circumstances, the intestinal immune system can distinguish between harmful and harmless substances. In cats with IBD, this regulatory mechanism becomes disrupted. The immune system mistakenly identifies normal substances as threats, triggering chronic inflammation of the intestinal lining.
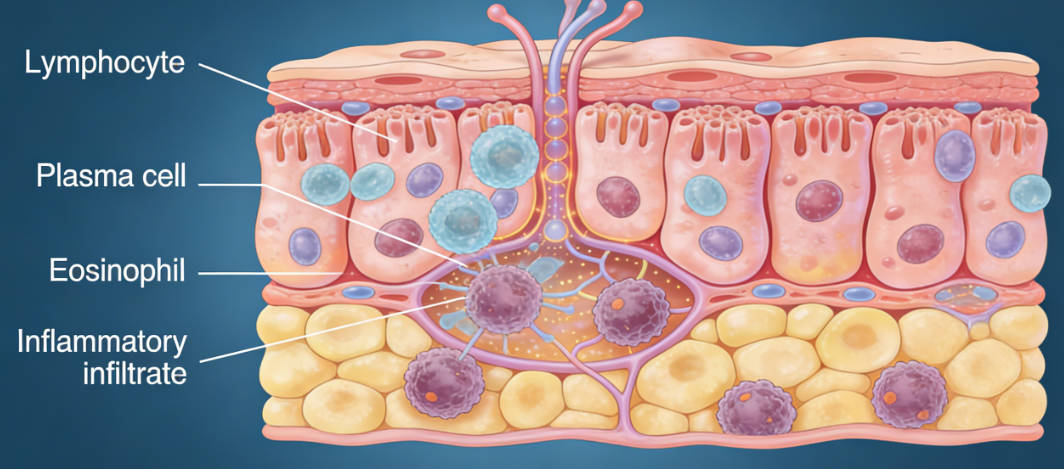
This inflammation persists over time and gradually affects the normal structure and function of the intestines. Inflammatory reactions lead to cellular infiltration of the intestinal mucosa, including lymphocytes, plasma cells, and eosinophils.
The accumulation of these inflammatory cells damages the intestinal lining and weakens its barrier function. Intestinal villi may become shortened or fused, reducing the surface area available for nutrient absorption. Inflammation also interferes with normal intestinal motility, further impairing digestion and absorption.
Common Clinical Signs
The clinical signs of feline IBD are usually chronic and non-specific. Because these symptoms overlap with many other chronic intestinal conditions, other causes must be ruled out first, such as intestinal parasites, medication side effects, exposure to plants or toxins, endocrine disorders, metabolic disease, or other gastrointestinal illnesses.

Gastrointestinal Signs:
Vomiting: Vomiting is one of the most common signs of feline IBD. Frequency can vary from occasional episodes to frequent vomiting in more severe cases. Typically, vomiting is chronic, occurring three or more times per week over a prolonged period (often several months). Vomitus may include undigested food, gastric fluid, bile, or occasionally blood-tinged material. Vomiting shortly after meals or foamy fluid on an empty stomach may both be associated with IBD.
Diarrhea: Diarrhea is another hallmark sign. Stool consistency may range from soft to watery, and some cats may pass stools containing mucus or blood. Frequency may increase to multiple bowel movements per day. Chronic diarrhea can lead to dehydration and further compromise overall health.
Soft stools: Some cats experience long-term soft stools with occasional blood, while appearing otherwise stable in general condition.
Constipation or altered defecation habits: Some cats may develop constipation, characterized by infrequent or dry stools. Others may show changes in defecation habits, irregular timing, or signs of discomfort and straining during bowel movements.
Signs Related to Poor Nutrient Absorption:
Weight loss: Chronic intestinal inflammation interferes with nutrient absorption, leading to gradual weight loss. Muscle mass and fat reserves decline, and the cat’s body contours become more pronounced. Even cats with normal or increased appetite may continue to lose weight because nutrients are not properly absorbed.
Poor coat quality: Malabsorption can result in a dull, rough, or brittle coat with increased shedding. Proteins, vitamins, and minerals are essential for healthy hair growth, and IBD disrupts their absorption.
Other Signs:

Changes in appetite: Some cats lose interest in food, while others may eat more but still lose weight. Appetite changes are influenced by intestinal inflammation affecting digestion and satiety signals.
Reduced activity and lethargy: Cats may appear tired, sleep more, and show less interest in play or interaction. Chronic inflammation and nutritional deficiencies can significantly reduce energy levels. In severe cases, cats may remain curled up in one place for extended periods.
Abdominal discomfort: Cats may show signs of abdominal pain, such as a hunched posture, tense abdominal muscles, or avoidance when the abdomen is touched. Vocalization or withdrawal during handling may also occur.
Why Does IBD Occur?
Feline IBD develops due to a combination of multiple factors rather than a single cause.
Immune Factors:
Immune dysregulation plays a central role in IBD. In affected cats, intestinal-associated lymphoid tissue becomes abnormally activated in response to gut microbiota or dietary antigens. This leads to excessive immune responses and inflammatory cell infiltration into the intestinal lining. These inflammatory cells release mediators that further amplify inflammation.
Autoimmune mechanisms may also contribute. Genetic or environmental influences may alter the antigenic properties of intestinal tissues, causing the immune system to recognize the cat’s own intestinal lining as foreign and attack it, resulting in chronic inflammation.
Genetic Factors:
Breed predisposition: Certain purebred cats, such as Siamese cats, appear to have a higher incidence of IBD, suggesting a genetic susceptibility.
Gene abnormalities: While specific genetic mutations have not been definitively identified in cats, studies in humans suggest that genes involved in immune regulation, intestinal barrier function, and microbiome stability may play a role. Similar mechanisms are suspected in feline IBD.
Environmental Factors:
Dietary factors: Food allergies or intolerances are significant triggers for IBD. Cats may react to certain proteins (such as chicken, beef, or dairy proteins), triggering immune-mediated inflammation. Food intolerance may also alter the intestinal environment and stimulate immune responses. Sudden diet changes or long-term feeding of low-quality diets containing poorly digestible ingredients or additives may further increase risk.
Stress-related factors: Cats are highly sensitive to environmental stress. Changes such as moving homes, introducing new pets, prolonged owner absence, or excessive noise can induce stress responses. Stress alters neuroendocrine function, affecting gut motility, secretion, and immune regulation, potentially triggering or worsening IBD.
Intestinal microbiome imbalance: A healthy gut microbiome is essential for intestinal health. Antibiotic use, infections, dietary changes, or parasitic infestations can disrupt microbial balance. Harmful bacteria may proliferate while beneficial microbes decline, weakening the intestinal barrier and promoting inflammation.
Diagnostic Evaluation and Treatment
Diagnostic Testing:
Basic blood work, including complete blood count and serum biochemistry, is essential. Findings may include mild liver enzyme elevation, abnormal globulin levels, or eosinophil changes.
Fecal examination helps rule out parasitic infections. Although these tests cannot definitively diagnose IBD, they are important for excluding other diseases with similar signs.
Abdominal ultrasound allows assessment of intestinal wall thickness and helps identify conditions such as pancreatitis or tumors that may not appear on blood tests.
Intestinal biopsy is the only definitive method for diagnosing IBD and determining severity. Biopsy samples are obtained via endoscopy or surgical procedures.
Treatment Approach:
Management of feline IBD focuses on controlling inflammation, alleviating symptoms, improving intestinal function, and maintaining adequate nutrition. Treatment typically involves dietary management, medication, and nutritional support.
Dietary modification includes elimination trials using novel or hydrolyzed protein diets, selecting easily digestible and low-allergen foods, and ensuring balanced nutrition. Feeding smaller, more frequent meals may reduce digestive burden.
Medical therapy may include anti-inflammatory medications, immune-modulating agents, antibiotics if secondary infections are present, and supportive gastrointestinal therapies. Probiotics and prebiotics may help restore intestinal microbial balance.
Nutritional supplementation, including vitamins and minerals such as vitamin B12 and folate, may be necessary in cases of malabsorption. In severe cases, assisted feeding or specialized nutritional support may be required.
Regular follow-up examinations are essential to monitor response to therapy and adjust treatment plans. Long-term management is often necessary to maintain symptom control and quality of life.
Conclusion
Feline inflammatory bowel disease is a chronic condition that typically requires long-term management rather than complete resolution. With appropriate dietary adjustments, medical support, and lifestyle management, most cats achieve good control of symptoms and maintain a satisfactory quality of life. Careful monitoring, high-quality nutrition, regular parasite prevention, and attention to food sensitivities can all help reduce the likelihood of disease progression and associated complications.


Comments (50)
Pet Lover
Great article! Very informative for pet owners.
Cat Parent
Thank you for sharing this helpful information!